The five-times sit-to-stand test (5XSTS) is a standardized geriatric tool developed to assess specific sit-to-stand transfers and lower extremity strength. It has the potential to predict mobility and fall risk. It is considered a functional test as it involves mobility consistent with functional activities of daily living. The test provides a method to quantify functional lower extremity strength and helps identify how patients complete transitional movements.
Many therapists have used the 5XSTS because it is quick to administer, requires little equipment, and requires very little space to perform. As a result, the 5XSTS has become a popular standardized test among healthcare providers to recognize those at substantial risk of recurrent falls, and more importantly, identify those who are appropriate for treatment and/or intervention before they fall.
How the 5XSTS Works
During the 5XSTS, the patient is asked to start in a seated position with their arms crossed. The patient is then asked to stand up and sit down five times in a row as fast as they can do so safely.
The patient should ascend and descend from a chair that is approximately 16 inches tall. The test is scored on the patient's age, sex, and the time it takes to perform the test.
Fall Risk and Cut-Off Scores
A cut-off score is the lowest value at which a certain status or category is attained on the 5XSTS. In this case, those who land within the cut-off scores are considered within normal function, and those outside are more at risk for falls.
Cut-off scores for the 5XSTS are calculated in seconds. This test has been studied for several decades in relation to fall risk, so specific cut-off scores may depend on the source that is cited.
Here is a complete list of normative data for the 5XSTS test based on age and sex, authored by Richard Wallace Bohannon:
- 20-29 years - 6.0±1.4 sec
- 30-39 years - 6.1±1.4 sec
- 40-49 years - 7.6±1.8 sec
- 50-59 years - 7.7±2.6 sec
- 60-69 years - 8.4±0.0 sec (male), 12.7±1.8 sec (female)
- 70-79 years - 11.6±3.4 sec (male), 13.0±4.8 sec (female)
- 80-89 years - 16.7±4.5 sec (male), 17.2±5.5 sec (female)
- 90+ years - 19.5±2.3 sec (male), 22.9±9.6 sec (female)
In addition to this research, Buatois et al., 2008 found that individuals with a score greater than 15 seconds had a 74%greater risk of recurrent falls than those who took less time, which can be seen in the chart below.
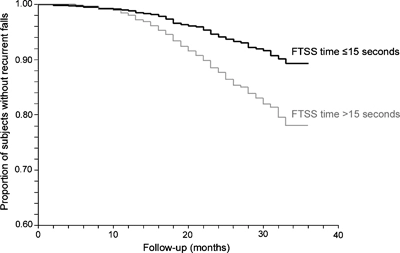
Minor Improvements = Big Impact
There is always room for improvement in the 5XSTS score and even minor changes can have a significant impact on the function and safety of a person. For this reason, patients and therapists should not be discouraged if a client/patient has a 5XSTS score well below the cut-off scores for fall risk. The 5XSTS is a screening or baseline measure that should be retested at a later date to help determine functional change. Even minimal changes in time can indicate an improvement in safety and function.
Subsequent test results should be monitored and correlated to the minimal clinical important change (MCIC) of the 5XSTS. MCIC is defined as the minimal change in the score that is clinically significant to produce a different outcome. An MCIC in the score will offer a noticeable improvement in function. Patients who can decrease their score by just 2.5 seconds can significantly improve function and fall risk.
5XSTS — More Than Just a Fall Risk
The 5XSTS measures functional lower limb muscle strength and may be useful in quantifying functional change of transitional movements. For instance, just by observing the quality of the movement, we can assess how much left or right lean is occurring when performing the activity. Asymmetrical leaning may indicate left- or right-side dominance. It could also potentially indicate painful compensatory patterns or unilateral ROM (range of motion) deficits. Meanwhile, strength and endurance are easily observed by determining if the person takes longer between each repetition in the test. Increased time between repetitions indicates endurance, strength, or cardiovascular difficulties within the person.
AI in Healthcare
By utilizing technologies like VSTBalance, clinicians can identify mobility deficits in older adults to determine if they are at risk of falling within the next 12 months. The system includes the 5XSTS assessment. By utilizing artificial intelligence, VSTBalance collects hundreds of data points including lateral lean and timed repetitions in the 5XSTS. These additional data points help clinicians determine the best course of treatment to improve overall function and stay healthy. Regular assessments with VSTBalance ensure that patient progression can be tracked with confidence.
.png)
.png)
.png)